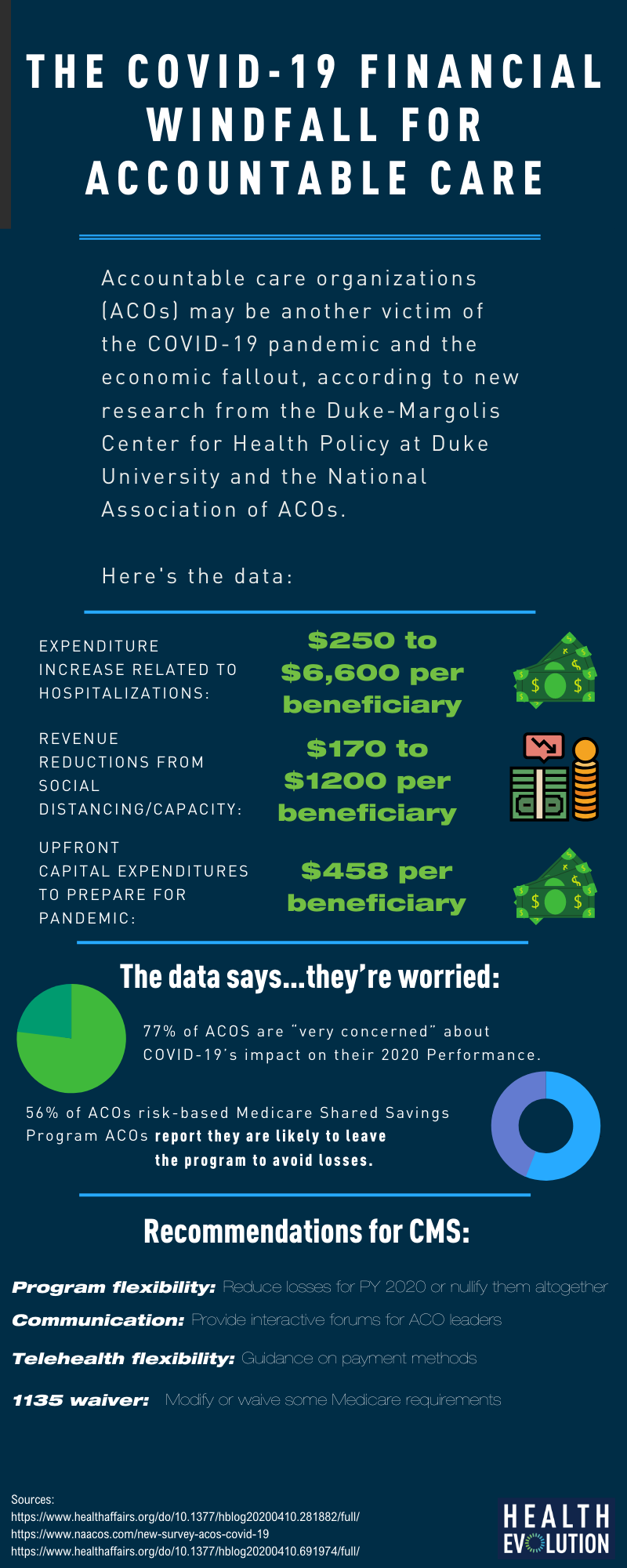
Accountable care organizations (ACOs) may be a victim of the COVID-19 pandemic and related economic fallout, according to new research from the Duke-Margolis Center for Health Policy at Duke University.
A Duke-Margolis research team, led by Mark McClellan, MD, Director, Duke-Margolis Center for Health Policy & Robert J. Margolis, M.D., looked at the financial impact COVID-19 could potentially have on ACOs, especially physician-led ACOs, in Health Affairs.
COVID-19: A turning point for AI regulation in health care
The researchers estimated ACOs could see increased per beneficiary per year expenditures of $250 if there is a low prevalence of COVID-19 cases in their attributed population to $6,600 per beneficiary per year if there is a high prevalence, just from a hospitalization standpoint. Physician-led ACOs could see revenue reductions, up to $1200 per beneficiary, thanks to social distancing and the cancellation of elective surgeries as well as an increase in upfront capital expenditures of personal protective equipment to prepare for the pandemic.
All told, these revenue losses and added expenditures could mean many ACOs in risk-based models are going to be operating at a loss. A new survey from the National Association of ACOs reveals that ACOs themselves understand that the financial impact of COVID-19 will be potentially devastating. Nearly 80 percent of ACOs say they are “very concerned” about the impact of COVID-19 on their ACO’s 2020 performance. Even more harrowing, almost 60 percent of respondents in risk-based models say they are likely to quit the Medicare Shared Savings ACO program to avoid financial losses.
According to the researchers at Duke-Margolis, “Medicare Shared Savings Program (MSSP) ACOs must decide before June 30 if they want to drop out of the program, or they will remain accountable for losses for the rest of the year.” Groups like NAACOs are calling on CMS to make the 2020 year a financial wash and not use this year’s data for assessing ACOs’ quality, beneficiary assignment, or shared savings or losses.
The Duke-Margolis researchers have made some recommendations to CMS as well. They say CMS should create an interactive virtual forum for all ACO leaders and providers and a “place to field questions well ahead of the June 30 deadline to drop out of the program or face downside risk.” They also say there is precedent and legislative language that would allow losses for PY 2020 during the emergency. The researchers also recommend further telehealth flexibilities and enacting a 1135 waiver to modify or waive some Medicare requirements.
Sources:
https://www.healthaffairs.org/do/10.1377/hblog20200410.281882/full/
https://www.naacos.com/new-survey-acos-covid-19
https://www.healthaffairs.org/do/10.1377/hblog20200410.691974/full/