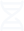The multi-year Health Evolution Forum brings together CEOs and other C-suite executives and subject matter experts to tackle the biggest challenges facing the industry today. This C-level collaboration across all health care sectors drives impactful near-term change, while identifying long-term needs.

Change Year-round
The Forum covers a wide range of evolving and emerging issues that are shaping the future of health care. These include topics related to Care Delivery Redesign, Payment Redesign, Community-Focused Health, Innovation and Discovery, Mental and Behavioral Health, and Organizational Transformation.
The influential and high-level thinking resulting from Forum discussions is captured and disseminated through white papers, consensus guidelines, and benchmarking tools to foster change across health care.
FORUM THOUGHT LEADERSHIP
Informal, Influential and
Invigorating Conversations
MEANINGFUL DISCUSSIONS
Roundtables
Roundtables represent an opportunity to inquire about, learn and influence discussions about current industry challenges, emerging solutions, and the future needs of health care. Because there are no boundaries associated with roundtable discussions, there are no limits to the impact these meetings have in shaping the future of health care.
Integrated Home-Based Care Models
How do we advance new models of home-based care that can deliver both episodic and longitudinal care delivery to patients with a wide range of needs?
LEARN MOREAchieving Consumer-Centric Care Experiences
How do we transform the consumer experience to rebuild trust and earn loyalty by confronting friction, fragmentation, and financial frustrations?
LEARN MOREValue-Based Care for Specialized Populations
How do leaders navigate the impact of policy changes and economic uncertainty on the value-based care landscape and identify opportunities for continued success and growth in value-based specialty care?
LEARN MORETransforming Health Care Economics
How can the health care ecosystem collaborate and innovate to achieve a more affordable and financially sustainable future?
LEARN MORECatalyzing Action to Advance Health for All
How do we accelerate and expand adoption of proven and emerging solutions to improve health outcomes, especially for those who are often overlooked or excluded?
LEARN MORELeading Coalitions for Healthy Communities
How do we build expansive alliances and effective partnerships to address the biggest challenges in community health—and what scalable solutions can we design together?
LEARN MOREAI and Data-Powered Innovation
How do we navigate the growing pace of innovation and realize the promise of AI in an ever-evolving business, policy, and technology landscape?
LEARN MOREPersonalized Health and Lifelong Wellness
How do we realize the promise of scientific and technological innovation to create a sustainable, proactive, person-centered ecosystem that delivers lifelong wellness?
LEARN MOREInnovations in Mental and Behavioral Health
How do we advance high-impact and evidence-based mental and behavioral health care models to better serve the unique needs of distinct patient populations?
LEARN MOREConfab for Advancing Women in Leadership
How do we achieve greater advancement of women in senior executive roles and expand their impact in addressing health care's most pressing challenges?
LEARN MOREFrontiers in Courageous Leadership
How do we lead our organizations through pivotal industry shifts and confront systemic challenges to truly meet the current and future needs of our businesses, workforce, and the people we serve?
LEARN MORETHOUGHT LEADERSHIP
Emerging Insights
Emerging Insights captures the real-time ideas, strategies, and solutions Health Evolution Fellows and guest experts surface through the dynamic, cross-industry conversations happening among C-suite executives and thought leaders in the Forum Roundtables.
From breakthrough innovations to bold leadership approaches, these insights reflect what’s top of mind for decision makers as they navigate complex challenges and shape the future of health care. Informed by the lived experiences and lessons of leaders across the ecosystem, Emerging Insights offers a window into the collaboration that’s driving industry progress.
Updated regularly, this collection is designed to inform, inspire, and spark continued innovation.
Explore what’s emerging—and what’s ahead.
Click on a Roundtable below to see takeaways from recent Forum Roundtable gatherings.
-last updated on June 27, 2025
AI AND DATA-POWERED INNOVATION
AI and Data-Powered Innovation
How do we navigate the growing pace of AI innovation and realize the promise of big data in an ever-evolving business, regulatory, and technology landscape? Learn More
• Effective AI governance faces a dual mandate for ethical innovation. As a starting place, leaders must validate technologies to ensure their underlying algorithms, inputs, and outputs are ethical. Leaders also must build the right training and guardrails to ensure the workforce uses AI outputs ethically. A robust governance structure should support both of these mandates.
• The new Trump administration has emphasized cultivating AI innovation in the private sector. Health care leaders have an opportunity to engage in bidirectional dialogue with policymakers on regulatory frameworks to achieve a balance between implementing guardrails for deploying AI safely in health care and driving forward progress. Health care leaders should lean in during this pivotal moment to guide the future of technological advancement.
• NEW!: Leaders should view AI as a catalyst for driving positive change in health care — not as a cure-all solution. Instead of looking at AI as a panacea for solving complex challenges such as prior authorization, leaders should look for ways they can integrate AI into systemic transformation efforts aimed at addressing inherent foundational issues in health care that can cause abrasion, delays, and potential patient harm.
DATA-DRIVEN HEALTH EQUITY STRATEGIES
Data-Driven Health Equity Strategies
How do we strengthen our commitment to advancing health equity and adopt proven solutions as we navigate emerging technologies and shifting challenges? Learn More
• Industry leaders are looking to invest in and launch bold initiatives to advance health equity through data-driven approaches that are proven to improve outcomes and generate ROI. Roundtable participants defined “bold” initiatives as those that:
– In addition to focusing on racial and ethnic disparities, target disparities among patients in rural and urban areas, people with disabilities, people of different income levels, and others who face challenges in health care.
– Enable new partnerships that can combat disparities among patient populations outside of Medicare and Medicaid, such as those enrolled in employer-sponsored health plans.
– Unlock data silos and bolster data accuracy, disaggregation, consistency, and completeness.
• While shifting societal attitudes and regulations can challenge efforts specifically focused on advancing health equity, health care leaders should remain committed to the fundamental work of improving quality outcomes. Prioritizing continuous quality improvement and data transparency can help organizations address health disparities, which in turn improves health, lowers overall health care costs, and drives community wellbeing.
• Headlines narrowly focus on how AI could perpetuate disparities, and health care leaders must ensure AI tools are built in ways that represent diverse populations to avoid perpetuating inequities. But executives shouldn’t miss the opportunity AI presents to prevent and address disparities, such as using AI to surface care gaps and help facilitate tailored solutions to reduce those gaps. Leaders must do both to maximize AI’s potential for positive impact.
• NEW!: Truly advancing health requires the health care ecosystem to move beyond acting for communities to acting with them. Health care leaders must shift from viewing collaboration and co-creation as a one-time step or crisis response to embedding and centering patients and communities as essential partners from the outset of—and throughout—their work. By purposefully and genuinely engaging communities, leaders can develop more effective solutions, build trust, and ensure participating communities meaningfully benefit from innovation.
DIGITAL-FORWARD CONSUMER EXPERIENCE
Digital-Forward Consumer Experience
How do we drive digital transformation and omni-channel strategies to improve consumer experience and business performance? Learn More
• The most challenging aspects of evaluating digital health innovations are measuring ROI and determining whether a digital solution will integrate into existing operations and delivery practices. Roundtable attendees said they increasingly are using both internal and external validation processes when evaluating digital solutions.
• A growing number of health care organizations are integrating behavioral science into their consumer engagement strategies, but often in narrow and siloed ways that fall short of meeting desired outcomes. To improve the effectiveness of these types of interventions, leaders should clarify their central goals, find the right behavioral science techniques to support those objectives, and root out complexity and conflicting incentives that undermine success.
• The digital health care landscape is saturated with point solutions that don’t fully meet the needs of either patients or providers. As a result, the market is demanding comprehensive platforms that converge point solutions into modular, scalable, and interoperable solutions that can meet holistic needs and integrate into existing systems. But for platformization to both emerge and succeed, health care leaders must be willing to prioritize necessary infrastructure updates to support implementation. In addition, leaders must collaborate with providers and patients to address the inherent frustration, distrust, and fatigue that’s resulted from their repeated experiences with ineffective solutions.
• The health care industry has reached a critical inflection point: with public trust in health care institutions at an all-time low and frustration at an all-time high, consumers are now actively turning away from incumbent health care institutions and seeking alternatives for information and care. Absent accepting accountability and taking decisive actions to rebuild trust, health care organizations risk further damaging their long-time standing as credible, influential pillars in their communities. Health care leaders must listen to consumers’ concerns, truly understand their needs, and build solutions that meaningfully improve consumers’ experience.
INNOVATIONS IN MENTAL AND BEHAVIORAL HEALTH
Innovations in Mental and Behavioral Health
How do we hold the ecosystem accountable for achieving equitable access and high quality in mental health care? Learn More
• Leaders must instill accountability and transparency across the entire care delivery ecosystem to effectively treat patients with substance use disorders and provide the long-term support patients need to remain in recovery. Integrating data from community organizations, PCPs, EDs, rehab centers, digital care providers, and others is essential to enable providers to identify patients at risk and/or patients who have relapsed, so they can connect those patients with the care and resources they need to continue their recovery and improve outcomes.
• In addition to deploying mental health-focused benefits and programs in the workplace, employers must equip managers with training and resources to support employee engagement with these tools. For initiatives to be successful, CEOs—as well as other trusted messengers—must champion mental health awareness to reduce stigma and ensure everyone throughout the organization prioritizes mental health and wellbeing.
• Innovators in mental and behavioral health often focus on scaling solutions at the national level, but there is significant opportunity to expand and improve care for patients with complex mental and behavioral health needs at the local level. Leaders can focus on forming partnerships with health care and community organizations at the local and state levels to create coordinated systems that provide the long-term, community-driven care and support essential for helping patients with complex needs achieve sustained recovery and thrive.
• NEW!: Successfully treating youth mental health requires creating a comprehensive network that spans across clinical, family, social, and educational settings. Effective models focus on reorienting from individual- to family-based care, expanding presence and partnership beyond traditional settings, integrating peer-support systems, and prioritizing evidence-based care models. Ultimately, these innovative approaches ensure patients can access and receive high-quality, holistic, longitudinal care that leads to long-term recovery and thriving.
INTEGRATED HOME-BASED CARE MODELS
Integrated Home-Based Care Models
How do we dvance new models of home-based care that can deliver both episodic and longitudinal care delivery to patients with a wide range of needs? Learn More
• Investors and innovators expect more investment in home-based care models, but with a broader application of how we decentralize care and focus on meeting patients where they are, which may include facilities outside the home. Companies should look to bring care to patients, not bring patients to care.
• PACE is poised for growth as the industry seeks new, effective ways to care for the country’s increasing senior population. But critical challenges inhibit PACE programs’ ability to scale, including a complex regulatory environment, a dearth of technological innovation to address the programs’ unique needs, barriers to collecting data that can help quantify PACE’s value, and a shortage of clinicians and leaders working in PACE. Innovators have an opportunity to collaborate with PACE organizations on solutions that can ease these barriers.
• While Hospital-at-Home and primary care models often get the most attention in the home-based market, there is increasing interest in scaling specialty care at home. Roundtable Fellows identified mental and behavioral health, musculoskeletal condition, and skilled nursing care as areas well poised for home-based expansion. To enable this growth, cross-industry leaders must work together to create tailored payment models that support value-based reimbursement and integrate these new services into the care continuum with bidirectional referral streams to ensure patients receive care in the settings that best meet their needs.
• NEW!: The range of ways AI can support home-based care is rapidly expanding. Beyond supporting providers in delivering care in the home, AI can also serve as critical connective tissue that orchestrates better coordination across sites of care, helps patients better engage in care from their homes, and harnesses the vast amount of non-clinical data generated in the home to improve and personalize patient care. To maximize AI’s potential in home care, innovators must partner with incumbent health care organizations and consumers to ensure tools integrate with existing systems and advance solutions providers and consumers will want, use, and trust.
LEADING COALITIONS FOR HEALTHY COMMUNITIES
Leading Coalitions for Healthy Communities
How do we strengthen our commitment to advancing health equity and adopt proven solutions as we navigate emerging technologies and shifting challenges? Learn More
• Employers are uniquely poised to address social factors impacting health given their many touchpoints with employees. Opportunities for employers to address these social needs include implementing programs focused on drivers of health and preventive care. Furthermore, employers can serve as a platform and partner externally to connect employees with other supplemental benefits, such as SNAP, in order to maximize support.
• Especially when navigating uncertainty, organizations working together as coalitions should come to the table with humility and trust, which includes being willing to challenge traditional power dynamics, recognizing when to lead and when to step back, and identifying who within the coalition is best positioned to drive meaningful change. Furthermore, coalition leaders must take active steps to nurture and maintain coalitions over time.
• With state funding and community health infrastructure facing significant changes, health care leaders can seek to fill gaps by forming coalitions that prioritize cross-sector collaboration; robust, trust-based partnerships; and financial innovation to enable initiatives aimed at supporting and improving community health. Leaders in these coalitions should strive to co-create responsive and effective solutions that drive wellbeing throughout the community to help ensure resiliency amid political, economic, and social uncertainty.
• NEW!: Health care leaders do not need to start from scratch—or work alone—when looking for solutions to boost community health, especially during times of scarce resources and limited capacity. Instead, leaders should look for opportunities to build coalitions with organizations seeking to scale high-value, but often underutilized, platforms that address shared challenges, such as PACE and collaborative care models. By aligning around proven solutions and forging innovative, cross-sector partnerships, leaders can maximize existing resources and platforms to accelerate transformation while shifting from reactive problem solving to proactive, solution-oriented impact.
PERSONALIZED HEALTH ECOSYSTEM
Personalized Health Ecosystem
How do we achieve widespread access to and adoption of breakthroughs in personalized prevention, diagnostics, therapeutics, and wellness? Learn More
• Employers can tailor benefits to meet their workforces’ specific needs and provide customized navigation services to stand out and advance personalized health. The navigation layer can transform uniform benefits into a personalized experience.
• Consumer technology companies are increasingly creating features that allow individuals to monitor their day-to-day health and wellness. As patients become more empowered in managing their health using data collected through direct-to-consumer technology, incumbent health care organizations recognize the need to collaborate with these companies on data sharing, workflow integration, and proving clinical and economic value.
• Consumers are looking for personalized, preventive approaches to health that span across their care journeys and lifetimes. To meet those heightened expectations, health care organizations can no longer operate in siloes. Leaders must collaborate with both health care incumbents and key partners beyond the traditional health system, especially to build innovative data systems that connect social and biological factors that influence health, as well as craft new payment structures that reimburse for long-term health outcomes and evolving care needs.
• NEW!: Gene therapies can transform patients’ lives by more effectively treating—or even curing—serious diseases, but patients’ access to gene therapies remains limited. To maximize the treatments’ potential, leaders across the health care ecosystem must shift their mindset from viewing gene therapies as isolated breakthroughs and embed them into the fabric of care delivery. Leaders will need to work collaboratively across industry, government, and patient communities to create trusted, scalable platforms for providing gene therapies by reimagining models for manufacturing, regulating, financing, delivering, and educating patients about these treatments.
TRANSFORMING HEALTH CARE ECONOMICS
Transforming Health Care Economics
How can the health care ecosystem collaborate and innovate to achieve a more affordable and financially sustainable future? Learn More
• The industry largely has focused on care model innovation to achieve sustainability and scalability in primary care. However, Roundtable Fellows believe the industry needs to focus on creating innovative business and payment models to truly unlock the power of primary care in a sustainable, scalable way. 70% of Roundtable attendees said they believe the best way to pay for primary care is through a capitated payment model with shared risk on total cost of care.
• While cost pressures and fiduciary responsibilities dominate headlines about the employer market, reducing health care spending isn’t employers’ exclusive goal. Employers want to prioritize services that provide high-quality outcomes and consumer experiences and support the workforce’s overall health and wellbeing. Employers increasingly are seeking partnerships with health care organizations to fundamentally shift how care is financed and delivered in ways that drive transparency and advance a more patient-centered approach.
• Many health system leaders view the transition to value-based payment with an “either-or” mindset, which can overshadow how value-based care delivery models can help drive success under both volume- and value-based incentives and hinder investments in care transformation. However, the clinical infrastructure that underpins total-cost-of-care models can also help maximize use of scarce high-cost capacity and support an over-extended workforce regardless of payment structures. Recognizing these “always-win opportunities” liberates leaders to accelerate care redesign efforts that enable success under both current and future economics.
• NEW!: The pharmaceutical and pharmacy sector has long operated with siloes and opacity, but mounting pressure from patients, policymakers, and industry stakeholders has forced a critical juncture: pharmaceutical and pharmacy leaders must take meaningful action to address access and affordability concerns or face intensifying regulation and competitive disruption. To ensure sustainability, pharmaceutical and pharmacy leaders must acknowledge their sector’s role in creating pain points and initiate bold partnerships across the health care ecosystem that will increase transparency.
VALUE-BASED CARE FOR SPECIALIZED POPULATIONS
Value-Based Care for Specialized Populations
What are the critical elements for succeeding under and scaling value-based specialty care models? Learn More
• Industry leaders expressed uncertainty about both the regulatory landscape and appetite for progression of value-based care for specialized populations. 55% of Roundtable participants said they were optimistic about the future of value-based specialty care, but 27% were neutral and 18% were pessimistic.
• The health policy landscape faces uncertainty as the new Trump administration and GOP-controlled Congress take charge, and near-term priorities will depend on key agency leadership and personnel decisions. Health care leaders have a critical opportunity to actively engage and influence policymakers to ensure continuing support and advancement of value-based care.
• NEW!: Payers and providers are moving away from deploying point solutions that are disconnected from their infrastructure and long-term strategic goals. Leaders are evaluating point solutions in the context of fit with desired financial and clinical outcomes, current payment models and risk arrangements, and existing technology systems. Baseline table stakes for partnership now include establishing shared goals and realistic expectations, ensuring strong data-sharing capabilities, and committing to iterative collaboration.
Enterprise Members
Premier Partner

Corporate Members
Interested in Joining?
The Forum’s peer-to-peer collaboration between health care leaders unlocks impactful solutions that enable near-term change. Don’t miss out on the powerful opportunities that Forum presents.
PARTNERSHIP
Corporate Membership Opportunities
Corporate Membership Opportunities:
Membership with Health Evolution opens a vast array of dynamic opportunities within the global health ecosystem.
This support helps health care leaders accelerate the mission of creating a more affordable and accessible, equitable and effective, proactive and personalized health sytem. Members benefit from high-level knowledge sharing in Forum Roundtables, in-person convenings, and published insights, leveraging the power of peer-to-peer dialogue.